Bipolar Hip
Bipolar Hip remains a cornerstone for femoral neck fracture management in busy African theatres. It is fast to teach, predictable for rotating teams, and compatible with geriatric pathways that prioritize early mobilization. When a solution reads like a pathway rather than a box of parts, committees trust it and lists stay calm.
Hospitals do not only evaluate components. They also judge whether a vendor can keep schedules reliable, documentation simple, and training repeatable. A disciplined Bipolar Hip program reduces cancellations, limits overtime, and improves the experience for patients and staff. This consistency turns first cases into steady routines.
Distributors seek stability as well. A price that seems low but depends on irregular freight or unclear labeling becomes expensive in practice. Ortonom Medical connects clinical method with logistics and service so the whole pathway stays predictable. Bipolar Hip benefits when every link in the chain is visible and owned.

Population needs also matter. As life expectancy rises, fracture services face sustained demand in both public and private networks. A clear Bipolar Hip program helps hospitals reserve total hip capacity for suitable indications while giving trauma teams a safe, efficient option that fits real conditions.
What Ortonom Medical delivers in Bipolar Hip systems
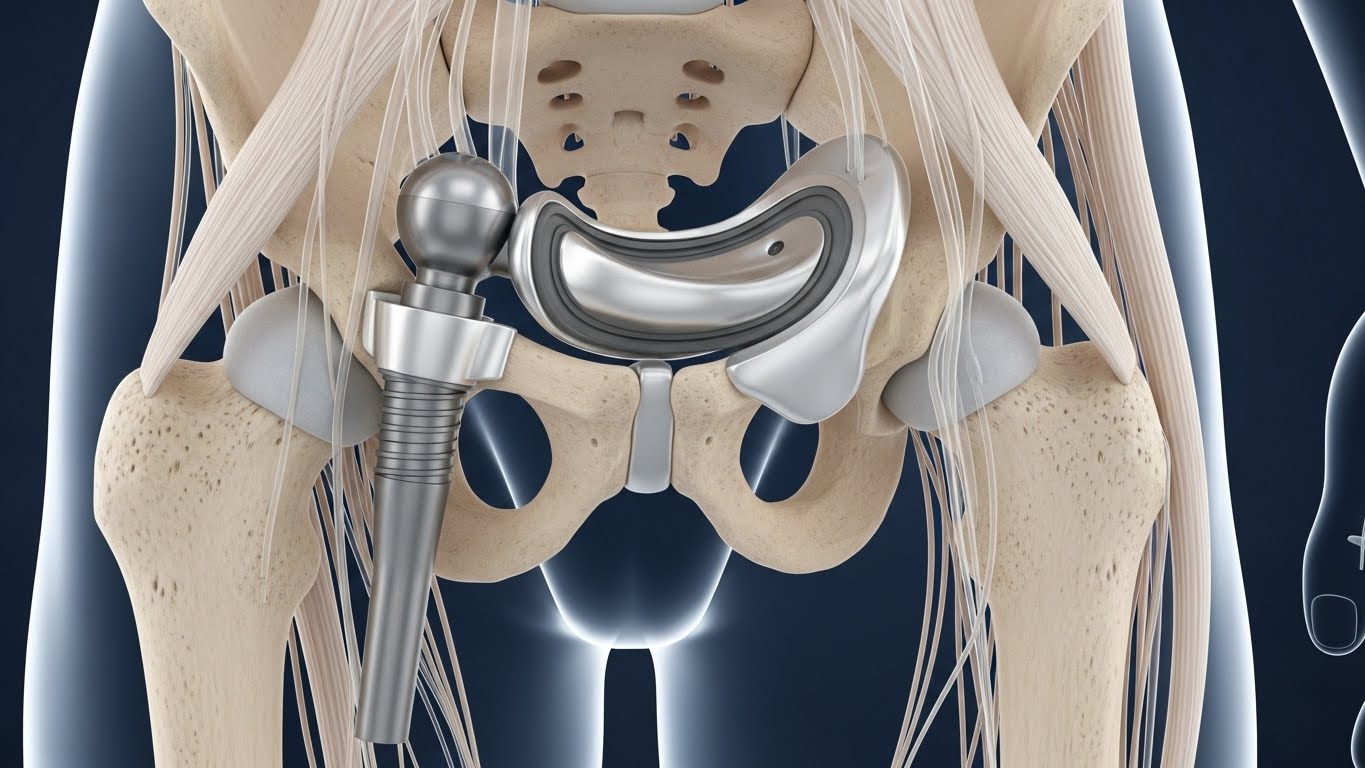
Ortonom Medical designs Bipolar Hip families to deliver stability, simplicity, and repeatability. Stem geometry supports axial and rotational control in osteoporotic bone while keeping a familiar broaching feel. This balance helps surgeons who move between trauma and elective lists maintain confidence and speed.
The bipolar head system is organized for quick, error resistant selection. Diameters are easy to read under pressure. The step between sizes is intuitive. Trial components mirror the final assembly so tactile feedback during reduction matches what the team will feel after implantation. This alignment reduces surprises.
Instrumentation follows the clinical sequence, not a catalog order. Canal entry, rasp progression, trial reduction, head selection, and final seating appear in the same order on the tray that the team will execute at the table. Handles and markings are legible with gloves and in low light. That clarity protects attention.
Documentation and labels respect committee expectations. Technical files trace design inputs through verification and validation to biocompatibility and shelf life. IFU come in English and French with QR links to concise clips. Labels scan quickly for UDI so perioperative teams spend time on patients, not on paperwork.
Surgical technique highlights for Bipolar Hip
Preoperative planning sets targets for length, version, and offset. A brief huddle aligns surgeon, scrub, and CSSD on tray layout and verification points. By starting with a shared mental model, the team prevents small misunderstandings from becoming late night delays.
Femoral canal preparation emphasizes gentle entry and controlled rasp progression in fragile bone. Version is confirmed deliberately before trialing. Trial reduction reconciles length and offset against the template rather than habit. This short, consistent loop protects stability and function.
Head selection is taught as a visible decision. The team confirms diameter, checks taper cleanliness, and rehearses reduction with the chosen size. A simple pocket checklist turns these steps into a habit. When everyone sees the same checkpoints, performance becomes steady.
Closure routines support early mobilization. Nursing notes and patient leaflets use the same sequence and words as the intraoperative story. When bedside explanations match theatre steps, families feel informed and staff handovers become smooth. The pathway feels coherent from incision to discharge.
Training approach that compresses learning curves
Hospitals buy confidence as much as components. Confidence grows when any trained professional can re enter the Bipolar Hip pathway after time away. This requires one message across every channel. The video, the quick card, and the tray tell the same story.
Short micro lessons beat long lectures on busy trauma days. Ortonom Medical provides focused clips on rasp seating feel, canal preparation in osteoporotic bone, taper hygiene, and reduction stability testing. Teams watch a module during setup and walk straight into the corresponding step. Learning moves into action.
Verification becomes reflex through repetition. Version check, length reconciliation, gentle varus valgus stress, and impingement sweep appear in the same order in all materials. When checks are short and visible, they are not skipped. The outcome is fewer revisions and calmer lists.
Postworkshop support closes the gap between theory and practice. Named clinical contacts remain reachable during the first quarter. Early case shadowing on site or remotely helps the team internalize the rhythm. Bipolar Hip then runs like a routine, not an event.
Regulatory and documentation that pass at first submission
Committees approve the clearest story. Ortonom Medical prepares conservative, complete packs for Bipolar Hip. Technical files cover specifications, risk management, verification and validation, shelf life, and labeling. The template is uniform across families so reviewers do not relearn structure for each submission.
IFU are bilingual and diagram the exact sequence on the tray. QR links point to short clips that staff can watch between cases. Tray checklists are written for CSSD adoption to prevent rebuilds. These details remove avoidable delays and keep launch dates credible.
Compliance continues after approval. Version controlled masters, named regulatory contacts, and written change notes flow from factory to distributor to hospital. This traditional discipline prevents customs surprises and keeps audits routine. Bipolar Hip stays on schedule because documents stay current.
Country copy is localized without changing the method. English and French are standard. Arabic summaries can support logistics or patient education where helpful. The pathway remains identical while communication matches local expectations.
Product and stocking snapshot for Bipolar Hip programs
The table frames discussion for procurement and clinical leadership. It does not replace clinical judgment. It keeps attention on pathway clarity, stock logic, and teachability so the team can decide with confidence.
| Family | System | Core features | Typical use cases | Training focus |
|---|---|---|---|---|
| OrtoHip | Bipolar Hip modular | Streamlined instruments, modular heads, intuitive size ladder | Femoral neck fracture and geriatric trauma | Head selection and length reconciliation |
| OrtoHip | Bipolar Hip monoblock option | Robust simplicity for very high volume emergency rooms | Damage control and low resource settings | Reduction stability and nursing routine |
| OrtoHip | Hybrid pathway | Press fit cup with cemented stem when indicated | Mixed bone quality or canal concerns | Cement discipline and impaction control |
| OrtoHip | Transition to total hip pathway | Shared instrument language across partial and total | Conversion when indicated | Planning and patient selection conversation |
Inventory and logistics that protect the schedule
Logistics should be quiet in the best sense. Fast movers live close to theatres. For Bipolar Hip that usually means common head diameters and mid range stem sizes staged in country. Long tail sizes rotate from regional hubs to preserve cash while maintaining availability. Rules are public so requests match reality.
Instrument turnaround reduces stress. CSSD aligned checklists and planned maintenance windows keep trays returning on time. A simple board shows tray status and cases covered. When tomorrow’s sets are ready today, the program feels professional and staff remain calm.
If customs or transport slow a lane, communication is early and concrete. A workable workaround beats a promise that shifts pressure downstream. Under promise and over deliver stays a classic principle that builds trust. Bipolar Hip benefits when logistics stay honest.
Consignment is a behavior agreement as much as a stock decision. The hospital commits to monthly reporting and the vendor commits to published reorder rules. Shelf age is reviewed and the long tail is rotated. Predictable movement protects budgets and schedules.
Ninety day launch plan that keeps promises
| Phase | Focus | What happens | Outcome |
|---|---|---|---|
| Weeks 1 to 3 | Prepare | Finalize decks and IFU. Confirm regulatory pack. Build starter stock. Reserve theatre slots. | Ready paperwork and clear story |
| Weeks 4 to 6 | Train | Workshops for surgeons and scrub teams. First Bipolar Hip cases supervised. Emphasis on verification. | Calm execution under supervision |
| Weeks 7 to 10 | Execute | Ten to twelve cases per site. Debriefs after each list. Tune head size distribution. Align CSSD maintenance. | Stable cadence and honest stock |
| Weeks 11 to 13 | Scale | Add one hospital. Publish outcomes summary and change log. Approach frameworks with references. | Repeatability and references |
A short readiness audit precedes week one. The team checks that QR links work in theatres, IFU and labels are approved for the country, and starter stock matches templated sizes. These small checks remove common causes of delay. The launch becomes a prepared routine, not an experiment.
During training the goal is to make verification automatic. The same three or four checks repeat until they are reflex. Tray labels and pocket cards reinforce the order. This discipline reduces variance and protects the schedule when volumes rise.
Execution focuses on cadence and feedback. Short debriefs capture issues early. Usage data adjusts reorder points publicly so everyone understands the rule. When decisions are visible, trust grows and surprises fade. The list becomes quiet.
Scaling is earned through references, not promises. A lighthouse site and a secondary site produce calm numbers. Frameworks respond to proof. Bipolar Hip shows its value by keeping schedules and delivering steady outcomes.
Roles and service levels so public claims match daily reality
| Item | Ortonom provides | Partner commits | Typical timeline |
|---|---|---|---|
| Regulatory dossier | Technical files, labels, IFU in EN and FR for Bipolar Hip | Local submission, tracking, committee presence | Five to fifteen business days per pack |
| Launch training | Workshops, videos, pocket cards | Venue, attendee coordination, refresher plan | Within thirty days after appointment |
| Instruments readiness | Tray checklists, sterilization guidance, maintenance plan | CSSD capacity and maintenance schedule | Pre launch and quarterly |
| Inventory policy | Stock matrix, reorder rules, consignment proposal | Safety stock and monthly reporting | At contract and monthly review |
| Field support | Case shadowing and troubleshooting | Case scheduling and structured feedback | First three to six months |
| Country copy | Bilingual brochures, listings, FAQ | Localization and response SLAs | Live at launch and quarterly updates |
Clarity prevents disappointment. When duties are visible, problems become tasks and tasks become outcomes. This level of precision calms committee discussions and protects relationships. Bipolar Hip thrives under predictable roles and measured service.
Named clinical and regulatory contacts remain available during the first quarter. Incident paths and on call windows are written into the plan. Maintenance windows are booked with CSSD. The program stops relying on exceptional effort and starts relying on good habits.
Quarterly reviews measure cadence, tray turnaround, incident resolution times, and forecast accuracy. When indicators stay inside agreed ranges, the program is doing its job. If an indicator drifts, the method is corrected first. Numbers follow method.
A short feedback channel extends this clarity. Training tweaks, label updates, and stock pivots are captured in a one page note. Transparency shows that the team learns without noise. Renewals become calm and scope can expand with confidence.
Country focus across Africa
South Africa rewards programs that respect audit culture. A lighthouse hospital in Gauteng followed by a secondary site in the Western Cape demonstrates repeatability. Bipolar Hip fits because verification steps and documentation align with established routines. References open doors to frameworks.
Egypt blends large public tenders with growing private groups. Bilingual packs and prudent lead times are decisive. Early CSSD involvement prevents tray rebuilds and protects cadence. The same assets support Morocco and Algeria where French copy and Arabic summaries reduce coordination friction.
Nigeria and Ghana value vendors who publish their method and keep it. Showing reorder points and the latest adjustments builds confidence. Kenya and Tanzania respond well to on site teaching for first cases and simple consignment rules for fast movers. Libya and Gabon appreciate named contacts and clear maintenance windows. Bipolar Hip gains acceptance when relationships are visible and promises are kept.

Central and East African partners in DRC, Ethiopia, Somalia, Sudan, Senegal, Namibia, Cameroon, and Guinea often start with a single site to anchor the story. The same pathway scales across borders because documents and trays do not change. Bipolar Hip becomes portable when every artifact is consistent and every role is clear.
Closing invitation
If you bring hospital access, field discipline, and a service first culture, Ortonom Medical will bring a Bipolar Hip program that is coherent to teach and complete to document. Together we can run first cases without noise and convert intentions into routines that last. This calm execution earns surgeon loyalty and keeps committees comfortable.
Schedule the first workshop and set the first supervised cases. Publish a short outcomes note that shows lessons learned in daylight. Expand to a second site with the same assets and cadence so scale remains predictable. This method protects budgets, clarifies roles, and builds a steady reputation.
Ortonom Medical is ready to share one page spec snapshots, bilingual IFU, and a starter stock matrix tailored to your case mix. Bipolar Hip then becomes your reliable trauma pathway across Africa, one quiet list at a time.




 Ortonomy refers to the study and application of principles related to the proper function and structure of systems, especially in biological or technological contexts. In medical terms, it often refers to the alignment and balance of body structures.
Ortonomy refers to the study and application of principles related to the proper function and structure of systems, especially in biological or technological contexts. In medical terms, it often refers to the alignment and balance of body structures.